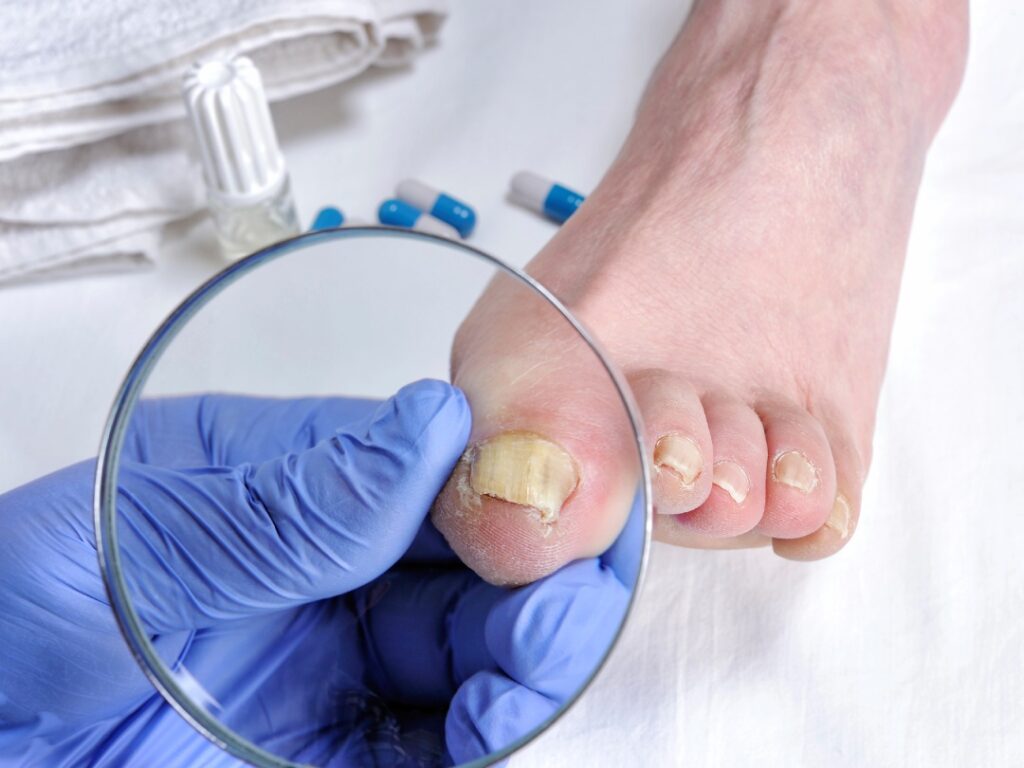
Living with diabetes means paying attention to parts of the body many people take for granted, and feet sit right at the top of that list. A small issue like an ingrown toenail may sound minor, yet diabetes can turn it into a serious medical concern.
Poor circulation, nerve damage, and slower healing change how the body responds to even tiny injuries. This article takes a deep dive into how diabetes affects ingrown toenails, why the risks increase, and how proper podiatric care protects long-term foot health.
Understanding Ingrown Toenails
An ingrown toenail develops when the edge or corner of a toenail presses into the surrounding skin instead of growing straight outward. This often happens on the big toe, though other toes can suffer as well. The condition causes redness, swelling, tenderness, and sometimes drainage. In people without diabetes, treatment may feel straightforward. For those managing diabetes, the situation requires more caution and expertise.
Ingrown toenails thrive in environments where pressure, moisture, and bacteria meet. Shoes, socks, and daily activity all influence how nails grow and interact with skin. Once the nail breaks the skin barrier, bacteria gain an entry point.
What Causes an Ingrown Toenail
Several everyday habits encourage ingrown toenails to form. Cutting nails too short leaves sharp edges that grow inward. Rounding the corners may look neat, yet it guides the nail straight into the skin. Tight shoes squeeze the toes together, forcing nails into surrounding tissue. Repetitive trauma, such as running or kicking sports, also increases risk.
Genetics play a role as well. Some people naturally grow curved or thick nails that resist straight trimming. For diabetics, nail thickness often increases over time, making trimming more difficult and increasing pressure along nail edges.
Early Warning Signs People Ignore
The earliest signs often feel mild. Slight redness, warmth, or tenderness near the nail edge may not raise concern. For people with diabetes-related nerve damage, these signals may not register at all. That lack of feedback delays action and allows the nail to continue digging into the skin. Swelling increases, bacteria multiply, and infection becomes more likely.
How Diabetes Changes Foot Health
Diabetes affects the body systemically, yet the feet often bear the brunt of long-term complications. Blood sugar levels influence circulation, nerve function, immune response, and skin integrity. Each factor plays a role in how an ingrown toenail develops and heals.
Blood Sugar and Circulation Issues
High blood sugar damages blood vessels gradually. Narrowed vessels reduce blood flow to the feet, which limits oxygen and nutrient delivery. Healing slows down, even for small cuts near the nail fold. Without proper circulation, the body struggles to fight infection effectively.
Reduced blood flow also means less swelling and redness in some cases, which can mask infection signs. A toe may look calm while trouble brews underneath the skin.
Nerve Damage and Reduced Pain Signals
Diabetic neuropathy affects sensory nerves in the feet. Tingling, numbness, or burning sensations often appear first. Over time, pain perception decreases. An ingrown toenail can worsen silently without triggering discomfort. By the time pain surfaces, infection may already spread into deeper tissue.
Why Minor Foot Problems Turn Serious
Poor circulation and nerve damage work together like faulty alarms and slow emergency responders. The body does not warn early, and when it finally reacts, healing moves sluggishly. This combination explains why diabetics face higher rates of foot ulcers, infections, and hospitalizations.
The Direct Link Between Diabetes and Ingrown Toenails
Diabetes does not directly cause ingrown toenails, yet it amplifies every associated risk. Nail and skin changes tied to diabetes create the perfect environment for complications.
Slower Healing and Infection Risk
Once an ingrown nail pierces the skin, bacteria take advantage of the opening. In diabetics, immune response weakens, giving bacteria more time to spread. Healing stalls, and infection may move into surrounding tissue or bone. What starts as localized redness can escalate into severe swelling, drainage, and odor.
Thickened Nails and Skin Changes
Many diabetics develop thick, brittle toenails due to fungal infections or metabolic changes. Thick nails press harder against skin and resist trimming. Dry skin and calluses crack more easily, offering additional entry points for bacteria. These factors raise the likelihood of recurring ingrown toenails.
Common Complications Diabetics Face With Ingrown Nails
Complications develop faster and progress further in diabetic feet. Ignoring an ingrown toenail invites serious consequences.
Infections That Spread Quickly
Bacterial infections in diabetic toes may advance rapidly. Redness spreads beyond the toe, warmth increases, and pus may appear. Fever and chills signal systemic involvement. Without prompt care, infection may reach bone, a condition known as osteomyelitis.
Ulcers and Tissue Breakdown
Constant pressure from an ingrown nail combined with infection can cause open sores beneath or beside the nail. These ulcers struggle to close due to poor circulation. Long-term wound care becomes necessary, and the risk of tissue loss rises.
When Ingrown Toenails Become a Medical Emergency
Not every ingrown toenail requires emergency care, yet certain signs demand immediate attention. Delaying treatment puts overall health at risk.
Signs You Should Never Ignore
Rapidly spreading redness, intense swelling, foul-smelling drainage, blackened skin, or increasing pain signal serious trouble. Fever combined with toe pain suggests infection spreading beyond the foot. These symptoms require urgent podiatric evaluation.
Vital Podiatry Cypress Foot and Ankle Specialist
Vital Podiatry Cypress Foot and Ankle Specialist provides comprehensive diabetic foot care focused on prevention, early intervention, and safe treatment. Specialized training allows podiatrists to manage ingrown toenails while protecting circulation and nerve health.
How Professional Care Prevents Severe Outcomes
Professional podiatric care addresses ingrown toenails before complications develop. Safe nail trimming, sterile techniques, infection control, and ongoing monitoring reduce the risk of ulcers and hospitalization. Customized treatment plans consider circulation status, nerve function, and overall health.
Safe Treatment Options for Diabetics
Treatment depends on severity, infection presence, and nail structure. A podiatrist selects the safest approach based on individual risk factors.
Conservative Treatments
Mild cases often respond well to professional nail trimming and pressure relief. Topical medications control bacterial growth, while proper footwear reduces irritation. Regular follow-ups ensure healing progresses smoothly.
Medical and Surgical Solutions
Recurrent or severe ingrown toenails may require partial nail removal. Modern procedures focus on precision and minimal trauma. In some cases, treatment prevents regrowth along the problematic nail edge, offering long-term relief.
What Not to Do at Home
Home remedies pose serious risks for diabetics. Digging into the nail with sharp tools, soaking in harsh chemicals, or attempting self-surgery can worsen the condition. Even small cuts invite infection. Professional care remains the safest option.
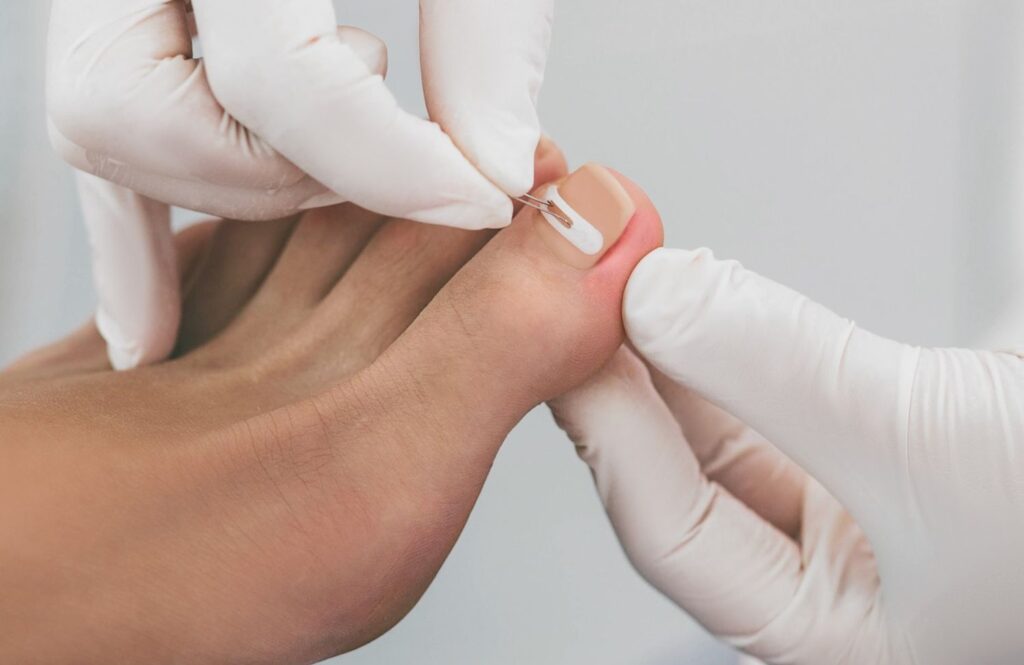
Preventing Ingrown Toenails When You Have Diabetes
Prevention protects mobility and quality of life. Consistent foot care habits make a major difference.
Nail Care Habits That Protect Your Feet
Trim nails straight across and keep them at moderate length. Avoid tearing edges or cutting too close to the skin. Professional trimming helps those with limited vision, flexibility, or hand strength.
Footwear Choices That Matter
Shoes with roomy toe boxes reduce pressure on nails. Breathable materials control moisture, while proper support distributes weight evenly. Avoid narrow or pointed shoes that compress the toes.
How Often Diabetics Should See a Podiatrist
Routine podiatric visits catch problems early. Many diabetics benefit from checkups every two to three months. Those with neuropathy, circulation issues, or previous ulcers may need more frequent care. Regular monitoring keeps small issues from becoming serious.
The Emotional Toll of Chronic Foot Pain
Chronic toe pain affects daily life in ways people often overlook. Walking becomes stressful, sleep suffers, and anxiety builds around potential complications. Reliable foot care restores confidence and supports independence.
Vital Podiatry Cypress Foot and Ankle Specialist Serving the Aberdeen Business Park Community and Beyond in Cypress
Vital Podiatry Cypress Foot and Ankle Specialist is dedicated to serving the diverse needs of the local community of Cypress, including individuals residing in neighborhoods like Aberdeen Business Park. With its convenient location near landmarks such as the Highland Grove Business Park and major intersections like Telge Rd. & Moray View Dr. (coordinates: 29.925868685885302, -95.64472829315025), we offer podiatrist ingrown toenail Cypress services.
Get Podiatrist Ingrown Toenail at Aberdeen Business Park Now
CALL US NOW!
(281) 937-4546
Navigate from Aberdeen Business Park to Vital Podiatry Cypress Foot and Ankle Specialist Now
Protecting Long-Term Foot Health Starts With Early Action
Diabetes magnifies the risks linked to ingrown toenails. A condition that seems minor can escalate quickly without expert care. Early treatment, preventive habits, and guidance from Vital Podiatry Cypress Foot and Ankle Specialist safeguard foot health and overall well-being. Healthy feet support mobility, comfort, and peace of mind.
FAQs
1. Can a diabetic ingrown toenail heal without treatment?
Healing without professional care rarely occurs due to circulation and immune challenges.
2. How quickly can infection develop in a diabetic toe?
Infection may progress within days once the skin barrier breaks.
3. Are ingrown toenails painful for diabetics?
Pain varies, as nerve damage often reduces sensation.
4. Should diabetics trim their own toenails?
Professional trimming lowers injury risk and ensures proper technique.
5. Can ingrown toenails lead to amputation?
Severe infection and untreated ulcers increase that risk significantly.