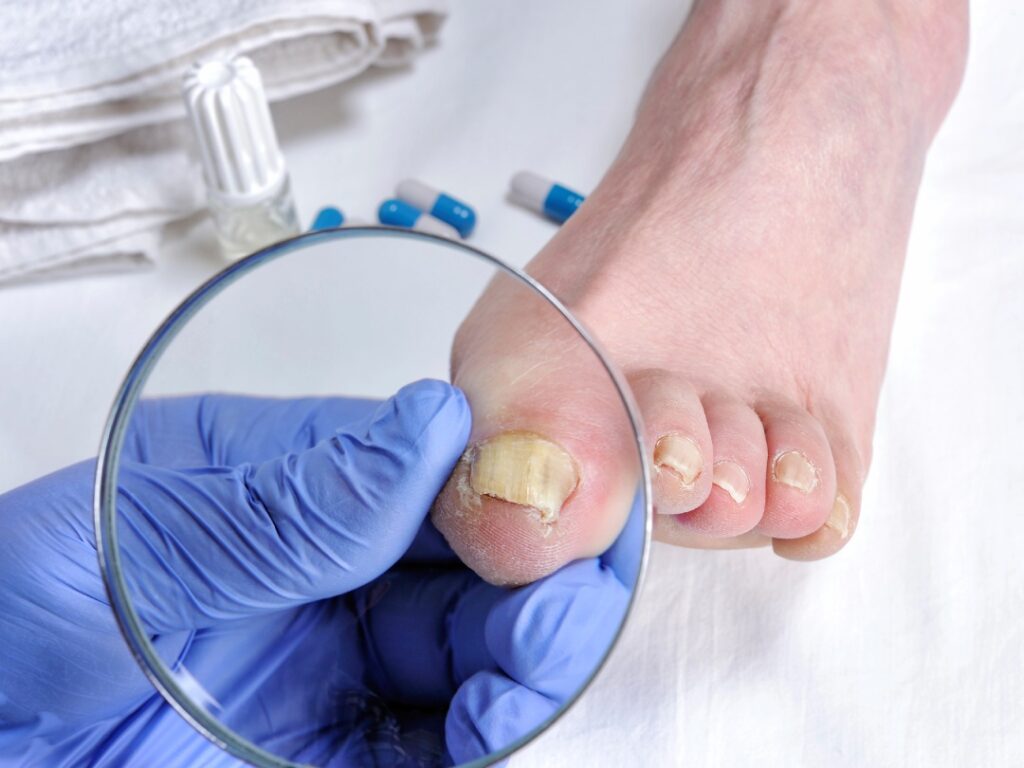
Understanding Diabetic Foot
What Is a Diabetic Foot?
A diabetic foot is a term used to describe foot problems that occur in people with diabetes. High blood sugar levels over time can damage nerves, blood vessels, and skin, making the feet more vulnerable to injuries, infections, and ulcers. It is not just one problem but a combination of several factors that gradually weaken the foot’s defenses.
Think of your foot like a house. Diabetes can quietly damage the foundation (nerves), block the plumbing (blood vessels), and make the walls (skin) fragile. At first, the damage is invisible, but eventually, small cracks—like tiny cuts or blisters—can become serious issues if left unchecked.
Why Diabetes Impacts the Feet
Diabetes affects the feet more than other parts of the body for two main reasons: circulation and nerves. Poor blood flow slows healing, while nerve damage (neuropathy) reduces the ability to feel pain or detect injuries.
Without feeling pain, even small cuts or pressure sores can go unnoticed. This silent progression is why diabetic foot problems often appear suddenly and severely. Maintaining awareness of your feet’s health is the first step to prevention.
Why Diabetes Makes Feet More Vulnerable
Diabetes affects the feet in two major ways: neuropathy and poor circulation. Nerve damage reduces the ability to feel pain, so you might step on a sharp object without realizing it. Reduced blood flow limits oxygen and nutrients reaching tissues, which slows healing.
Feet are particularly at risk because they are far from the heart. Gravity, tight shoes, and daily stress increase pressure points, which combined with diabetes, accelerates foot problems.
Early Warning Signs of Diabetic Foot
Recognizing early signs is key to preventing serious complications. Here are common symptoms that indicate the beginnings of diabetic foot issues:
Numbness and Tingling
Tingling, burning, or numbness in the feet can signal nerve damage. Peripheral neuropathy often starts subtly, with occasional pins-and-needles sensations, but it can worsen over time. Ignoring these signs is risky because numbness can hide injuries like cuts or blisters, allowing them to worsen unnoticed.
Changes in Skin Color and Temperature
Noticeable color changes in the foot—such as redness, dark spots, or pale areas—may indicate reduced blood flow. Similarly, cooler feet can be a warning sign of poor circulation. These changes often occur before ulcers or infections appear.
Slow Healing Wounds
Even minor scrapes, cuts, or blisters that take longer than usual to heal can be a red flag. High blood sugar levels impair the body’s healing ability, and wounds that linger may quickly escalate into ulcers or infections.
The Role of Nerve Damage
Peripheral Neuropathy Explained
Peripheral neuropathy is a condition where nerves outside the brain and spinal cord are damaged. In diabetics, this primarily affects the feet. Neuropathy reduces sensation, so the foot cannot effectively detect pain, temperature changes, or pressure.
How Neuropathy Starts
Nerve damage begins gradually. Persistently high blood sugar levels damage the tiny blood vessels that supply nerves with oxygen and nutrients. Over time, this causes nerve fibers to malfunction.
High Blood Sugar and Nerve Function
Excess glucose in the blood triggers chemical reactions that harm nerve fibers. Think of it as sugar coating tiny wires inside your foot. Slowly, these wires stop transmitting signals correctly, leading to numbness, tingling, or burning sensations.
Common Neuropathy Symptoms in Feet
- Tingling or burning sensations
- Loss of vibration or temperature sensitivity
- Weakness in foot muscles
- Cramping or stabbing pain
These symptoms may appear gradually and worsen if blood sugar levels remain uncontrolled.
Circulatory Problems and Blood Flow
Peripheral Artery Disease in Diabetics
Poor circulation is another major contributor to diabetic foot problems. Peripheral artery disease (PAD) narrows blood vessels, reducing blood flow to the feet. Without adequate oxygen, tissues heal slowly, making infections more dangerous.
Signs of Poor Circulation in Feet
- Cold or pale feet
- Weak pulse in the ankles or feet
- Hair loss on toes or legs
- Shiny or thin skin
PAD combined with neuropathy increases the risk of developing serious foot ulcers and infections.
Infections and Ulcers
How Minor Injuries Become Serious
Because diabetic feet often have reduced sensation and circulation, minor injuries can escalate quickly. A small blister, scratch, or ingrown toenail can become an open wound. Bacteria thrive in these environments, leading to infections that are hard to treat.
Signs of Infections in the Foot
- Swelling and redness around wounds
- Pus or foul odor
- Warmth around the affected area
- Fever or chills in severe cases
Prompt treatment is crucial. Ignoring infections can result in gangrene and, in worst cases, require amputation.
Risk Factors for Developing Diabetic Foot
Several factors increase the likelihood of developing foot problems if you have diabetes.
How Minor Injuries Escalate
In diabetics, minor injuries like blisters, cuts, or ingrown toenails can escalate quickly. Neuropathy masks the pain, and poor circulation slows healing. Bacteria can enter the wound, leading to infection that spreads beneath the skin.
Poor Blood Sugar Control
Persistent hyperglycemia is the biggest risk factor. High blood sugar levels accelerate nerve and blood vessel damage, making injuries and infections more likely.
Smoking and Lifestyle Choices
Smoking reduces blood flow, which directly impacts healing. Combined with poor diet, sedentary lifestyle, or alcohol consumption, it amplifies the risk of diabetic foot complications.
Footwear and Foot Care Habits
Tight, ill-fitting shoes can cause pressure points and blisters. Skipping daily foot checks or neglecting proper hygiene can allow small problems to escalate. Wearing breathable, supportive shoes and inspecting feet daily can prevent many issues.
Vital Podiatry Cypress Foot and Ankle Specialist: Prevention and Care
Professional care plays a crucial role in managing diabetic foot risk. Vital Podiatry Cypress Foot and Ankle Specialist provides specialized evaluation, treatment, and education to prevent complications.
Routine Foot Exams
Regular foot exams help detect early signs of neuropathy, circulation problems, or infections. Podiatrists can identify issues invisible to the untrained eye and recommend interventions before problems worsen.
Professional Treatments and Interventions
Depending on the stage of damage, treatments may include:
- Custom orthotics to relieve pressure
- Wound care and infection management
- Surgical interventions for severe cases
- Guidance on blood sugar management and foot hygiene
Early intervention saves not only feet but overall mobility and quality of life.
Daily Foot Care Tips to Avoid Diabetic Foot
Cleaning and Moisturizing Feet
Wash feet daily with lukewarm water and mild soap. Dry thoroughly, especially between toes, to prevent fungal infections. Use a moisturizer to prevent cracks, but avoid applying it between toes.
Inspecting Feet Daily
Check feet daily for cuts, blisters, redness, or swelling. Use a mirror if needed. Early detection allows prompt treatment before minor injuries worsen.
Choosing Proper Footwear
Wear well-fitted shoes with adequate cushioning. Avoid tight or pointed shoes that create pressure points. Socks should be soft, clean, and moisture-wicking to reduce friction and bacterial growth.
When to Seek Medical Help
Warning Signs That Require Immediate Attention
Seek prompt medical care if you notice:
- Open wounds or ulcers that do not heal
- Severe swelling or redness
- Signs of infection (pus, odor, warmth)
- Sudden changes in skin color or temperature
How Early Intervention Saves Limbs
Early treatment prevents infections from spreading and reduces the risk of amputation. Podiatrists can provide wound care, prescribe medications, and guide safe lifestyle practices that protect your feet.
Vital Podiatry Cypress Foot and Ankle Specialist Serving the Oak Cliff Place Community and Beyond in Houston
Vital Podiatry Cypress Foot and Ankle Specialist is dedicated to serving the diverse needs of the local community of Houston, including individuals residing in neighborhoods like Oak Cliff Place. With its convenient location near landmarks such as the Cypress Falls High School and major intersections like US-290 Frontage Rd. & Huffmeister Rd. (coordinates: 29.9258696, -95.62916320000001), we offer diabetic wound care doctor Cypress services.
Get Diabetic Wound Care Doctor Services at Oak Cliff Place Now
CALL US NOW!
(281) 937-4546
Navigate from Oak Cliff Place to Vital Podiatry Cypress Foot and Ankle Specialist Now
Protecting Your Feet: Steps to Prevent Diabetic Complications
Diabetic foot begins quietly but progresses quickly if unnoticed. It starts with high blood sugar affecting nerves and circulation, then worsens with minor injuries and poor healing. Awareness, daily foot care, and professional evaluation—like the services provided by Vital Podiatry
Cypress Foot and Ankle Specialist—are critical to preventing serious complications. Protecting your feet is protecting your mobility and independence, and it begins with attention to small changes before they become big problems.
FAQs
1. Can diabetic foot develop without pain?
Yes, neuropathy can reduce sensation, so injuries may go unnoticed until severe.
2. How often should a diabetic check their feet?
Daily self-inspection is recommended, with professional foot exams at least once a year.
3. Are infections the main complication of diabetic foot?
Infections are common, but ulcers, gangrene, and reduced mobility are also major complications.
4. How does blood sugar control affect foot health?
Maintaining normal blood sugar levels slows nerve and vascular damage, reducing the risk of foot problems.
5. When should I see a podiatrist?
See our podiatrist immediately if you notice wounds, redness, swelling, numbness, or signs of infection. Regular check-ups are also recommended for prevention.