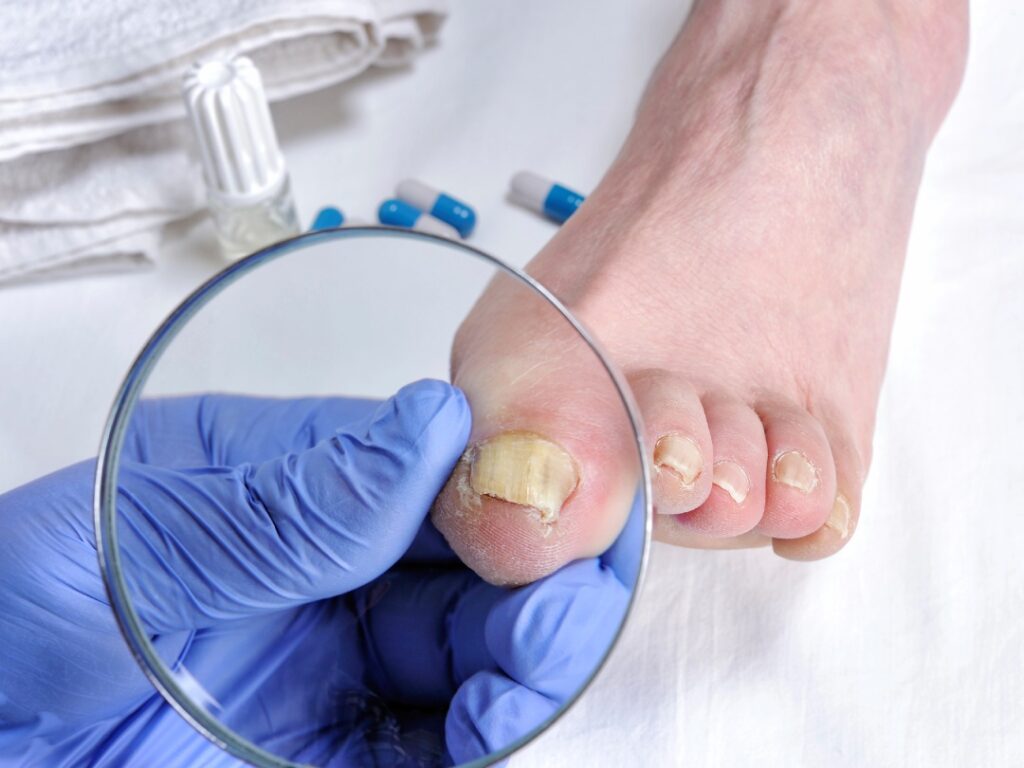
Diabetic foot ulcers can feel like an endless struggle. If you have diabetes, the idea of a wound that refuses to heal can be frightening, and you might wonder if complete recovery is even possible. The truth is, diabetic foot ulcers can heal fully with the right care, early intervention, and ongoing management.
Healing is rarely instant, but with proper treatment and lifestyle adjustments, patients can regain healthy skin, avoid complications, and reduce the risk of recurrence. In Houston, many patients turn to specialized clinics such as Vital Podiatry Foot and Ankle Specialist, where expert care improves healing outcomes and overall foot health.
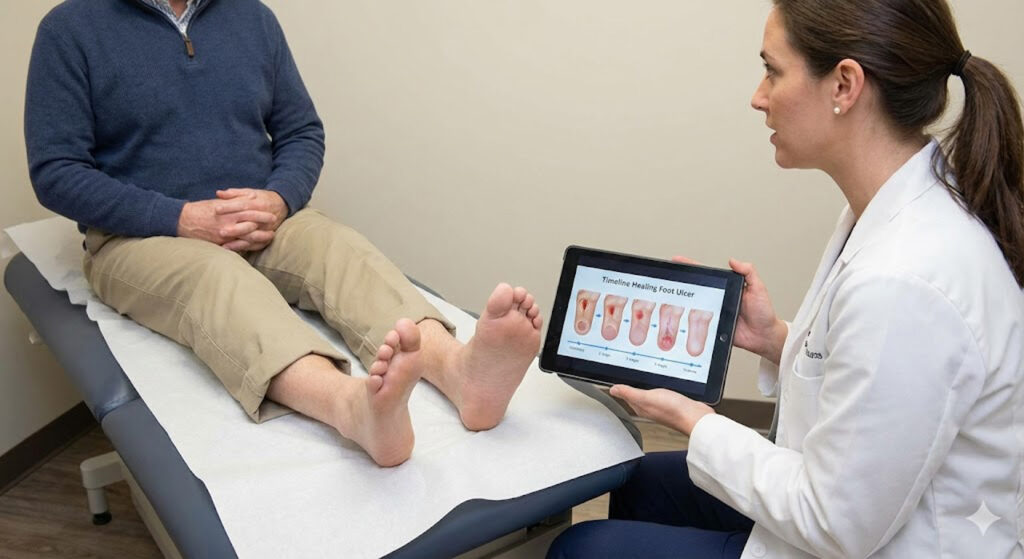
Understanding Diabetic Foot Ulcers
Diabetic foot ulcers are open sores or wounds that typically develop on the bottom of the foot, toes, or heels. They occur due to a combination of high blood sugar, poor circulation, and nerve damage. Left untreated, these ulcers can worsen, lead to infections, and sometimes even threaten the foot itself. Understanding how they develop helps patients take the right steps toward complete healing.
What Causes Diabetic Foot Ulcers?
Diabetic foot ulcers rarely appear out of nowhere. Several factors contribute to their development:
- Neuropathy (Nerve Damage): Diabetes can damage nerves, especially in the feet, making it hard to feel pain or discomfort. Minor injuries like a cut or blister can go unnoticed and develop into ulcers.
- Poor Circulation: High blood sugar can affect arteries, reducing blood flow. Without proper circulation, oxygen and nutrients fail to reach damaged tissue, slowing healing.
- High Blood Sugar: Elevated glucose levels weaken immune response and impair the body’s ability to repair tissues.
- Foot Deformities: Bunions, hammer toes, or abnormal gait patterns increase pressure points, making certain areas of the foot more prone to ulcers.
Common Symptoms and Warning Signs
Early detection dramatically increases the chances of healing. Watch for these signs:
- Persistent redness or swelling
- Open sores that do not heal within a few days
- Discharge, pus, or unusual odor
- Blackened tissue or dark spots
- Tingling, numbness, or burning sensations in the foot
If you notice any of these, immediate care is crucial to prevent further damage and infection.
Risk Factors That Delay Healing
Healing diabetic foot ulcers isn’t just about treating the wound itself. Overall health and lifestyle play a critical role. Several risk factors can make ulcers stubborn or slow to heal.
Poor Circulation and Neuropathy
Adequate blood flow is essential for tissue repair. When arteries are narrowed due to diabetes-related vascular disease, the body struggles to deliver nutrients and oxygen to the wound site. Neuropathy worsens the problem because patients may not feel pain, allowing wounds to worsen unnoticed.
Infection and Contamination
Open wounds are vulnerable to bacteria. Even minor infections can spread quickly, increasing inflammation and delaying healing. Severe infections may reach the bone, causing osteomyelitis, which requires aggressive treatment.
Lifestyle and Blood Sugar Control
Consistently high blood sugar slows tissue repair and immune response. Smoking, poor diet, and sedentary habits further complicate healing. Controlling glucose, maintaining a healthy diet, and staying active significantly improve the chances of recovery.
Stages of Diabetic Foot Ulcer Healing
Understanding the healing stages helps set expectations and highlights the steps needed to support recovery.
Early Stage: Inflammation and Infection Control
During the first stage, the ulcer is often red, swollen, and sometimes painful. The focus is on:
- Cleaning the wound regularly
- Preventing bacterial infections
- Protecting surrounding skin from further damage
Prompt care at this stage prevents ulcers from worsening and sets the foundation for regeneration.
Intermediate Stage: Tissue Regeneration
In this phase, new tissue forms, typically pink and fragile. Healing can stall if the area is exposed to pressure, friction, or contamination. Proper dressing, moisture balance, and offloading techniques ensure the tissue grows without interruption.
Advanced Stage: Wound Closure and Scar Formation
The final stage involves closing the wound and forming scar tissue. While healed, the area may remain more delicate than surrounding skin. Continuous protection and monitoring are essential to prevent recurrence or breakdown under stress.
How Treatments Impact Healing
Professional care significantly accelerates healing and prevents complications. Medical specialists employ a combination of strategies to tackle ulcers effectively.
Role of Podiatry Specialists
Podiatrists specialize in foot care, addressing not only ulcers but also the underlying causes like neuropathy and poor circulation. They provide guidance on foot care, wound management, and prevent future injuries, increasing the likelihood of complete healing.
The Vital Podiatry Foot and Ankle Specialist Approach in Windfern Forest, Houston
At Vital Podiatry Foot and Ankle Specialist, Houston patients receive personalized treatment plans. Their approach includes:
- Thorough wound assessment and monitoring
- Advanced debridement to remove dead tissue
- Offloading devices to reduce pressure
- Infection prevention strategies
- Collaboration with endocrinologists for optimal blood sugar control
This comprehensive approach maximizes the chance of full healing while minimizing recurrence.
Dressings, Debridement, and Offloading Techniques
Debridement removes dead tissue to promote healthy growth. Specialized dressings maintain moisture, protect against bacteria, and reduce friction. Offloading, using special shoes or braces, relieves pressure, allowing tissue to repair efficiently.
Advanced Therapies: Growth Factors and Hyperbaric Oxygen
For persistent ulcers, advanced therapies can jumpstart healing:
- Growth Factors: Stimulate cell proliferation and tissue repair.
- Hyperbaric Oxygen Therapy: Saturates tissues with oxygen, enhancing healing and fighting infection.
These treatments are especially helpful when conventional care fails to produce results.
Home Care Strategies to Promote Healing
Healing extends beyond the clinic. Patients must actively participate in care routines to ensure success.
Daily Foot Inspections
Checking your feet every day catches small issues before they become major problems. Look for cuts, blisters, redness, swelling, or drainage. Use a mirror if needed or ask a caregiver for help.
Maintaining Healthy Blood Sugar Levels
Consistent glucose management speeds up tissue repair. Monitor blood sugar regularly and follow diet and medication plans advised by your healthcare provider.
Proper Footwear and Pressure Relief
Wear diabetic-friendly shoes that distribute pressure evenly. Avoid walking barefoot to prevent injuries. Socks should be clean, dry, and free of tight elastic that could restrict blood flow.
Complications That Can Hinder Complete Healing
Certain complications make healing more difficult and require urgent attention.
Recurrent Ulcers
Scar tissue from previous ulcers is often weaker and more prone to breakdown. Offloading and protective footwear are essential to prevent recurrence.
Gangrene and Amputation Risks
Severe infections, tissue death, or uncontrolled blood sugar can lead to gangrene. In extreme cases, partial amputation may be necessary to save the foot or leg. Early intervention and professional care are crucial to prevent these outcomes.
Prevention and Long-Term Care
Preventing ulcers is easier than treating them. Long-term care focuses on protecting the feet and addressing underlying risk factors.
Routine Check-Ups and Monitoring
Regular visits to a podiatrist allow early detection of small issues. Imaging, lab tests, and vascular assessments identify problems before they become serious.
Lifestyle Habits That Reduce Recurrence
Maintaining blood sugar control, staying active, following foot care routines, and avoiding smoking reduce the risk of new ulcers and support ongoing healing.
Vital Podiatry Foot and Ankle Specialist Serving the Windfern Forest Community and Beyond in Houston
Vital Podiatry Foot and Ankle Specialist is dedicated to serving the diverse needs of the local community of Houston, including individuals residing in neighborhoods like Windfern Forest. With its convenient location near landmarks such as the Clark Henry Park and major intersections like W Sam Houston Pkwy N & Philippine St (coordinates: 29.88565,-95.54672), we offer diabetic foot care treatment services.
Get Diabetic Foot Care Treatment at Windfern Forest Now
CALL US NOW!
(281) 937-4546
Navigate from Windfern Forest to Vital Podiatry Foot and Ankle Specialist Now
Achieving Complete Recovery from Diabetic Foot Ulcers
Complete healing of diabetic foot ulcers is achievable with early detection, professional care, and proactive lifestyle habits. Patients in Houston benefit from specialized clinics like Vital Podiatry Foot and Ankle Specialist, where expert guidance, advanced wound care, and personalized treatment plans maximize healing chances.
By staying vigilant and following medical advice, diabetic foot ulcers can transform from a chronic concern into a fully manageable condition.
FAQs
1.How long does it take for a diabetic foot ulcer to heal?
Healing time varies depending on the size, location, and severity of the ulcer. Small ulcers may heal in weeks, while larger or infected wounds can take several months.
2.Can diabetic foot ulcers recur after healing?
Yes. Scar tissue is weaker and may break down under pressure. Protective footwear and careful monitoring help prevent recurrence.
3.What home care practices support healing?
Daily foot inspections, proper footwear, blood sugar management, and keeping wounds clean are essential for faster and safer healing.
4.When should I see a podiatrist?
Persistent sores, redness, swelling, drainage, or blackened tissue require immediate podiatric attention.
5.How does Vital Podiatry Foot and Ankle Specialist help patients in Houston?
We offer personalized treatment plans, advanced wound care, offloading strategies, infection management, and continuous monitoring to ensure the best chance for full healing.