Heel pain can sneak up on you in ways you don’t expect. One day you’re walking comfortably, and the next morning the first step out of bed feels like stepping on a sharp stone. For many people, this discomfort is caused by plantar fasciitis—a common yet frustrating condition that affects the bottom of the foot.
What makes plantar fasciitis tricky is that it often develops gradually. At first, the pain may appear only after long walks or workouts. But over time, even everyday activities like standing, cooking, or walking to the car can become uncomfortable.
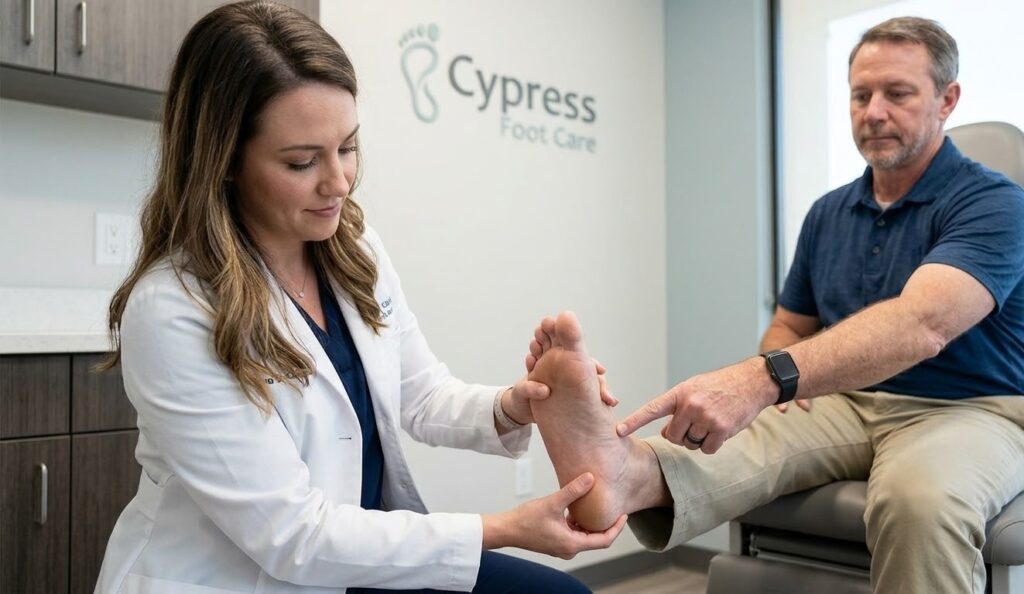
That’s where a foot and ankle specialist comes in. These medical professionals focus specifically on diagnosing and treating conditions affecting the feet and ankles. Through specialized knowledge, advanced tools, and personalized treatment plans, they can help relieve pain and restore mobility.
For individuals living near Meadows Of Northwest Park, understanding how a specialist approaches plantar fasciitis treatment can provide reassurance—and a clear path toward recovery.
Understanding Plantar Fasciitis
What Is Plantar Fasciitis?
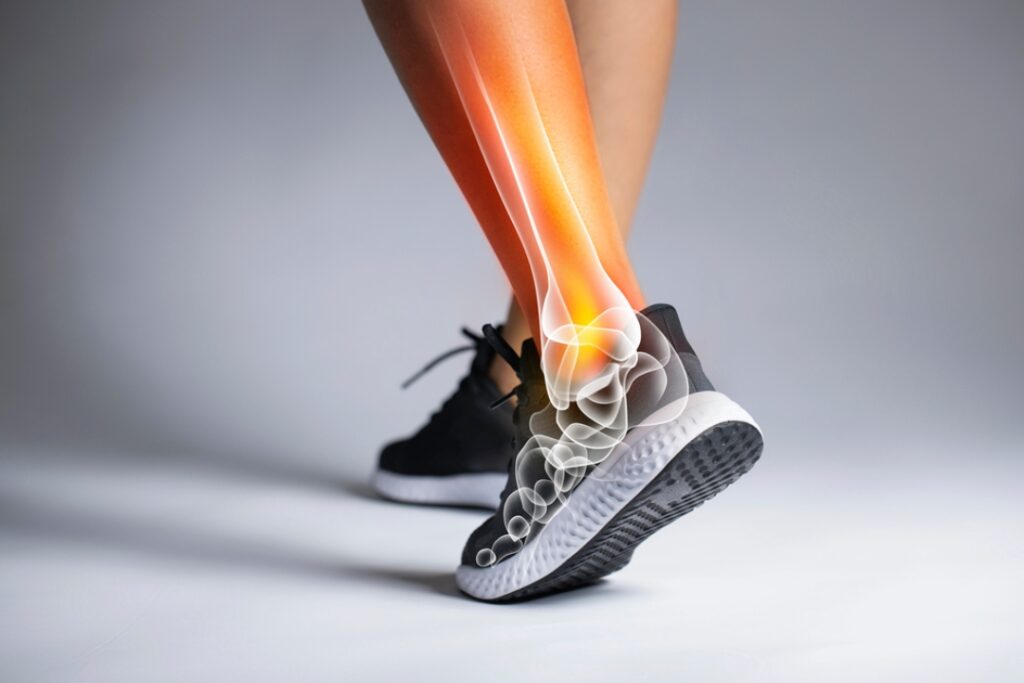
Plantar fasciitis occurs when the plantar fascia becomes inflamed or irritated. The plantar fascia is a thick band of connective tissue that runs along the bottom of the foot, stretching from the heel bone to the toes.
You can think of the plantar fascia as a built-in shock absorber. Every time you take a step, it supports the arch of your foot and helps distribute pressure evenly across the foot. Without this structure, walking or running would place extreme stress on the bones and joints.
However, when the plantar fascia is overworked or overstretched, small microscopic tears can develop. These tears cause inflammation, stiffness, and pain—particularly in the heel area.
Why Heel Pain Happens
Heel pain associated with plantar fasciitis usually develops because the tissue cannot keep up with the physical demands placed on it.
Imagine repeatedly bending a rubber band. At first, it stretches easily. But after enough tension, the rubber band weakens and begins to fray. The same concept applies to the plantar fascia.
When the tissue experiences repeated stress without sufficient recovery time, inflammation develops and pain appears.
Common Causes of Plantar Fasciitis
Overuse and Strain
One of the most common triggers for plantar fasciitis is repetitive strain. Activities that involve running, jumping, or extended walking place continuous pressure on the plantar fascia.
Athletes are particularly vulnerable, especially runners who train on hard surfaces. However, even everyday activities like long walks or standing for hours can create gradual strain on the foot.
Improper Footwear
Shoes play a larger role in foot health than many people realize. Wearing unsupportive footwear can dramatically increase the risk of plantar fasciitis.
Shoes without proper arch support or cushioning force the plantar fascia to absorb more impact than it should.
Common footwear problems include:
- Flat sandals without support
- Worn-out athletic shoes
- High heels that change foot alignment
- Minimalist shoes without cushioning
Lifestyle and Occupation
Certain jobs and lifestyles increase the likelihood of developing plantar fasciitis.
People who work on their feet for long periods—such as teachers, retail employees, nurses, or warehouse workers—place constant pressure on the heel.
Walking or standing on hard surfaces like concrete also increases the risk.
Early Warning Signs of Plantar Fasciitis
Morning Heel Pain
The most common symptom of plantar fasciitis is sharp heel pain during the first steps in the morning.
During sleep, the plantar fascia tightens slightly. When you step out of bed and place weight on the foot, the tissue stretches suddenly—causing pain.
Many people say it feels like stepping on a nail or sharp stone.
Pain After Long Periods of Standing
Pain may also appear after long periods of standing or walking.
For example, someone who spends an entire workday on their feet may notice worsening heel pain by the evening.
Tightness in the Foot Arch
Many individuals experience stiffness in the arch of the foot.
This tightness can create a pulling sensation along the bottom of the foot, especially after exercise or prolonged inactivity.
Why Seeing a Foot and Ankle Specialist Matters
Accurate Diagnosis
Heel pain is not always caused by plantar fasciitis. Conditions such as nerve compression, tendon injuries, or stress fractures may produce similar symptoms.
A foot and ankle specialist carefully evaluates the foot to determine the exact cause of the pain.
Preventing Long-Term Damage
Without treatment, plantar fasciitis may lead to chronic pain and altered walking patterns.
People often shift their weight to avoid heel pain, which can cause problems in the knees, hips, or lower back.
Early treatment helps prevent these complications.
Diagnostic Process Used by Specialists
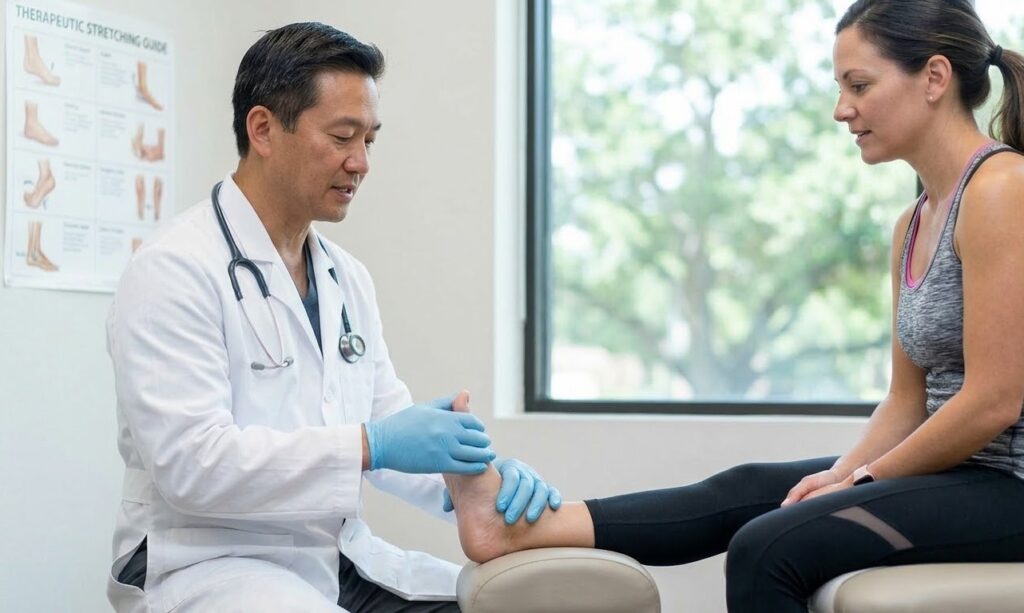
Physical Examination
During a consultation, a foot and ankle specialist performs a detailed examination of the foot.
This typically includes:
- Checking areas of tenderness
- Evaluating foot arch structure
- Testing flexibility and movement
- Observing how the patient walks
Imaging and Advanced Testing
If necessary, imaging tests may be used to confirm the diagnosis or rule out other conditions.
X-rays or Ultrasound
X-rays can detect bone abnormalities like heel spurs or fractures. Ultrasound imaging allows specialists to examine inflammation within the plantar fascia.
Conservative Treatment Methods
Most plantar fasciitis cases respond well to non-surgical treatment.
Rest and Activity Modification
Resting the foot allows the plantar fascia to heal. Specialists often recommend reducing high-impact activities like running or jumping.
Lower-impact exercises such as swimming or cycling may be recommended during recovery.
Custom Orthotics
Custom orthotics are specialized shoe inserts designed to support the unique structure of a patient’s foot.
They help:
- Stabilize the arch
- Distribute pressure evenly
- Reduce strain on the plantar fascia
Stretching and Physical Therapy
Stretching exercises improve flexibility in the plantar fascia and surrounding muscles.
Physical therapy may include:
- Calf stretching exercises
- Foot mobility training
- Strength-building routines
- Balance exercises
These therapies help restore normal foot function.
Advanced Treatments for Persistent Cases
When conservative treatments do not provide relief, advanced therapies may be recommended.
Corticosteroid Injections
Corticosteroid injections help reduce inflammation and provide temporary pain relief for severe cases.
Shockwave Therapy
Shockwave therapy uses sound waves to stimulate healing in damaged tissue.
This treatment encourages increased blood flow and tissue repair.
Minimally Invasive Procedures
In rare cases, minimally invasive procedures may be used to release tension in the plantar fascia.
These procedures typically involve shorter recovery times than traditional surgery.

The Role of Proper Footwear
Choosing Supportive Shoes
Supportive footwear is essential for both treatment and prevention.
The best shoes include:
- Good arch support
- Cushioning
- Firm heel support
Avoiding Flat or Worn-Out Shoes
Flat shoes without support can worsen heel pain. Similarly, worn-out shoes lose their ability to absorb impact.
Replacing athletic shoes regularly helps maintain foot support.
Preventing Plantar Fasciitis from Returning
Daily Stretching
Stretching keeps the plantar fascia flexible and reduces the risk of reinjury.
Maintaining Healthy Weight
Excess body weight increases pressure on the feet and heels.
Maintaining a healthy weight reduces strain on the plantar fascia.
Foot Strengthening Exercises
Strengthening exercises improve foot stability and arch support.
Examples include toe curls, towel scrunches, and resistance band exercises.
Vital Podiatry Foot and Ankle Specialist Serving Meadows Of Northwest Park
Residents of Meadows Of Northwest Park experiencing heel pain can benefit from expert podiatric care.
Personalized Care for Heel Pain
At Vital Podiatry Foot and Ankle Specialist, treatment plans are tailored to each patient’s specific needs.
Specialists evaluate lifestyle, activity level, and medical history to create an effective recovery plan.
Community-Focused Foot Health
Serving the Meadows Of Northwest Park community, the clinic emphasizes prevention, patient education, and long-term foot health.
Their goal is to help patients return to comfortable movement and daily activities.
When to Schedule an Appointment
Signs You Need Professional Care
You should consider seeing a specialist if:
- Heel pain lasts more than two weeks
- Walking becomes difficult
- Pain worsens with activity
- Home remedies do not help
Early treatment often leads to faster recovery.
Vital Podiatry Foot and Ankle Specialist Serving the Meadows Of Northwest Park Community and Beyond in Houston
Vital Podiatry Foot and Ankle Specialist is dedicated to serving the diverse needs of the local community of Houston, including individuals residing in neighborhoods like Meadows Of Northwest Park. With its convenient location near landmarks such as the Epps Island Elementary School and major intersections like Tomball Pkwy and Bammel North Houston Rd (coordinates: 29.91757,-95.49233), we offer foot and ankle specialist Houston services.
Get Foot and Ankle Specialist Services at Meadows Of Northwest Park Now
CALL US NOW!
(281) 937-4546
Navigate from Meadows Of Northwest Park to Vital Podiatry Foot and Ankle Specialist Now
Conclusion
Plantar fasciitis may begin as a mild discomfort, but it can quickly interfere with daily life if left untreated. Fortunately, foot and ankle specialists offer a range of treatments that address both the symptoms and the underlying cause of heel pain.
Through accurate diagnosis, personalized treatment plans, and preventive care, patients can regain mobility and enjoy daily activities without persistent pain.
For residents of Meadows Of Northwest Park, seeking care from Vital Podiatry Foot and Ankle Specialist can provide the expert support needed to restore comfort and long-term foot health.
FAQs
1. What is the fastest way to relieve plantar fasciitis pain?
Rest, stretching exercises, ice therapy, and supportive footwear are often effective first steps.
2. How long does plantar fasciitis take to heal?
Recovery may take several weeks to several months depending on the severity.
3. Are orthotics necessary for plantar fasciitis?
Custom orthotics provide arch support and help reduce stress on the plantar fascia.
4. Can plantar fasciitis return after treatment?
Yes, but maintaining good footwear, stretching regularly, and strengthening the feet can reduce the risk.
5. Is surgery common for plantar fasciitis?
Surgery is rare and usually considered only when conservative treatments fail.